What is a pressure ulcer definition
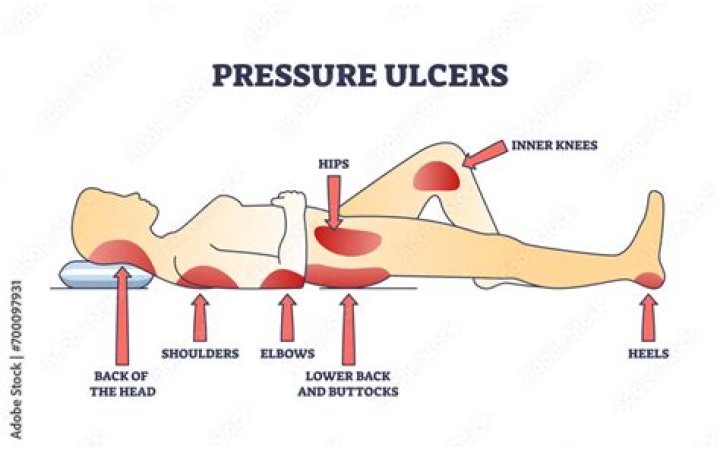
Bedsores — also called pressure ulcers and decubitus ulcers — are injuries to skin and underlying tissue resulting from prolonged pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such as the heels, ankles, hips and tailbone.
What is a pressure ulcer and how are they classified?
an open wound or blister – a category 2 pressure ulcer. a deep wound that reaches the deeper layers of the skin – a category 3 pressure ulcer. a very deep wound that may reach the muscle and bone – a category 4 pressure ulcer.
What are the 4 causes of pressure ulcers?
- being unable to move around easily due to old age or illness.
- weight loss – you may have less padding over bony areas.
- sliding down in a bed or chair – pressure on the skin cuts off blood supply because the skin is being pulled in different directions (called shearing)
What are the 4 stages of pressure ulcers?
- Stage 1 Pressure Injury: Non-blanchable erythema of intact skin.
- Stage 2 Pressure Injury: Partial-thickness skin loss with exposed dermis.
- Stage 3 Pressure Injury: Full-thickness skin loss.
- Stage 4 Pressure Injury: Full-thickness skin and tissue loss.
How do you describe an ulcer?
An ulcer is a sore on the skin or a mucous membrane, accompanied by the disintegration of tissue. Ulcers can result in complete loss of the epidermis and often portions of the dermis and even subcutaneous fat. Ulcers are most common on the skin of the lower extremities and in the gastrointestinal tract.
Are pressure sores painful?
It may feel warm to the touch. It may burn, hurt, or itch. The pressure sore may look blue or purple in people who have dark skin.
Is a DTI a pressure ulcer?
DTI has been recently added by the National Pressure Ulcer Advisory Panel as a separate category in the staging of pressure ulcers. There is currently a lack of consensus on how to identify and treat DTI, but preventive measures typically employed in the management of all pressure ulcers have been recommended.
Can bedsores lead to death?
Stage 4 bedsores can lead to life-threatening infections. Bedsores cause over 60,000 deaths each year according to the Agency for Healthcare Research and Quality (AHRQ) and are often the tragic result of nursing home neglect.Is Vaseline good for bed sores?
You can use any mild ointment, such as antibiotic cream or petroleum jelly (Vaseline). This will prevent the skin from becoming dry and will also protect the sore from dust, dirt, flies and other insects. Be careful not to rub or massage the skin around the pressure sore.
How do nurses prevent pressure ulcers?Prevention includes identifying at-risk persons and implementing specific prevention measures, such as following a patient repositioning schedule; keeping the head of the bed at the lowest safe elevation to prevent shear; using pressure-reducing surfaces; and assessing nutrition and providing supplementation, if needed …
Article first time published onHow do pressure ulcers affect patients?
People with grade four pressure ulcers have a high risk of developing a life-threatening infection. The characteristics are: Full thickness skin loss with extensive destruction, tissue necrosis, or damage to muscle, bone, or supporting structures, for example, tendon or joint capsule.
Where do pressure ulcers occur?
Bedsores — also called pressure ulcers and decubitus ulcers — are injuries to skin and underlying tissue resulting from prolonged pressure on the skin. Bedsores most often develop on skin that covers bony areas of the body, such as the heels, ankles, hips and tailbone.
What are the 3 types of ulcer?
- arterial ulcers.
- venous ulcers.
- mouth ulcers.
- genital ulcers.
How are pressure ulcers stages?
Stage 1 ulcers have not yet broken through the skin. Stage 2 ulcers have a break in the top two layers of skin. Stage 3 ulcers affect the top two layers of skin, as well as fatty tissue. Stage 4 ulcers are deep wounds that may impact muscle, tendons, ligaments, and bone.
What causes pressure sores on feet?
Pressure ulcers are sores that occur when pressure cuts off the blood supply to the skin. Stress caused by the body’s weight and the impact of striking the ground place the ball of the foot, the big toe, and the heel at the greatest risk. Left untreated, an ulcer may allow infection to enter your body.
Can an RN stage a pressure ulcer?
“Nurses cannot diagnose pressure ulcers.” In isolation that is true, but they can identify a wound as a pressure ulcer. This is supported by the National Pressure Ulcer Advisory Panel (NPUAP) and the American Nurses Association.
What is a Category 2 pressure ulcer?
A grade 2 pressure ulcer is defined as partial-thickness skin loss involving the epidermis, dermis or both. The ulcer is superficial and presents clinically as an abrasion or blister (Figure 2).
What is Kennedy terminal ulcer?
A Kennedy terminal ulcer is a skin wound that appears in some people during their final weeks of life. The term “Kennedy terminal ulcer” was first used in 1989. It’s also known as a Kennedy ulcer.
What is the fastest way to get rid of bed sores?
Bedsores are wounds that form due to prolonged pressure on the skin. The fastest way to get rid of bedsores is to relieve the pressure, keep the wound clean, take antibiotics and to employ other strategies. Bedsores are wounds that develop over several days or months due to prolonged pressure on the skin.
What is the fastest way to heal a pressure ulcer?
If the affected skin isn’t broken, wash it with a gentle cleanser and pat dry. Clean open sores with water or a saltwater (saline) solution each time the dressing is changed. Putting on a bandage. A bandage speeds healing by keeping the wound moist.
Do bed sores heal?
Once a bedsore develops, it is often very slow to heal. Depending on the severity of the bedsore, the person’s physical condition, and the presence of other diseases (such as diabetes), bedsores can take days, months, or even years to heal. They may need surgery to help the healing process.
Do bedsores smell?
Symptoms: The sore looks like a crater and may have a bad odor. It may show signs of infection: red edges, pus, odor, heat, and/or drainage. The tissue in or around the sore is black if it has died.
What does a Stage 1 pressure sore look like?
STAGE 1. Signs: Skin is not broken but is red or discolored or may show changes in hardness or temperature compared to surrounding areas. When you press on it, it stays red and does not lighten or turn white (blanch).
Which ointment is best for bed sores?
- alginate dressings – these are made from seaweed and contain sodium and calcium, which are known to speed up the healing process.
- hydrocolloid dressings – contain a gel that encourages the growth of new skin cells in the ulcer, while keeping the surrounding healthy skin dry.
What do pressure ulcers look like?
It can look like a scrape (abrasion), blister, or a shallow crater in the skin. Sometimes this stage looks like a blister filled with clear fluid. At this stage, some skin may be damaged beyond repair or may die. During stage 3, the sore gets worse and extends into the tissue beneath the skin, forming a small crater.
What happens when a bedsore goes to the bone?
A bed sore could lead to osteomyelitis if a bacterial infection enters the bone tissues. The most common causes of osteomyelitis are injuries or surgeries that put the patient at risk of an infection in the bloodstream.
What do bedsores look like?
Bedsores occur in stages: Stage 1 has unbroken, but pink or ashen (in darker skin) discoloration with perhaps slight itch or tenderness. Stage 2 has red, swollen skin with a blister or open areas. Stage 3 has a crater-like ulcer extending deeper into the skin.
How often should patients be turned?
Changing a patient’s position in bed every 2 hours helps keep blood flowing. This helps the skin stay healthy and prevents bedsores. Turning a patient is a good time to check the skin for redness and sores.
What antibiotics are used for pressure ulcers?
Amoxicillin-potassium clavulanate is a naturally occurring beta-lactam structurally similar to the penicillin nucleus. This antibiotic group of beta-lactam/beta-lactamase combination has demonstrated a broad-spectrum activity; therefore, it is frequently used for the treatment of infected pressure ulcers.
Where on the body do such ulcers most commonly occur?
Peptic ulcers are open sores that develop on the inside lining of your stomach and the upper portion of your small intestine. The most common symptom of a peptic ulcer is stomach pain. Peptic ulcers include: Gastric ulcers that occur on the inside of the stomach.
Does Medicare pay for pressure ulcers?
White-Chu noted, because the Medicare payment guidelines state that physicians must document pressure ulcers that are present on admission. Otherwise, Medicare will not pay the treatment costs of any pressure ulcers that progress to stage III or IV during hospitalization.



