Why is cardiac muscle sensitive to calcium
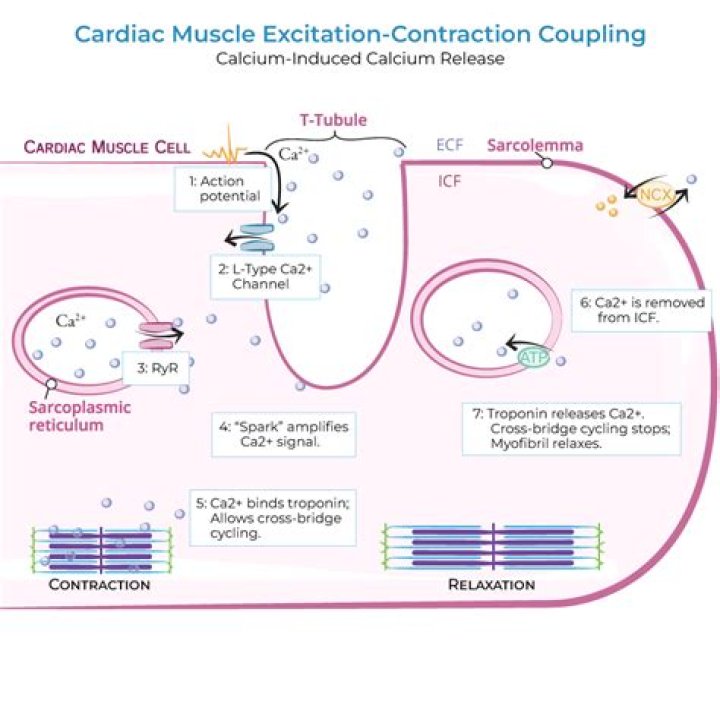
Myofilament proteins work in conjunction to allow the cardiac muscle to contract and relax in response to changes in intracellular free calcium ion concentration. Therefore, it is not surprising that genetic mutations in many of the myofilament proteins impact calcium sensitivity.
Why is calcium important for cardiac muscle?
Calcium particles enter the heart muscle cells during each heartbeat and contribute to the electrical signal that coordinates the heart’s function. Calcium particles also bind to machinery within the cell that helps the cell to squeeze together (“contract”), which makes the heart pump blood.
What causes calcium release in cardiac muscle?
Muscle Contraction and Actin-Myosin Interactions: Skeletal muscle contracts following activation by an action potential. Binding of Acetylcholine at the motor end plate leads to intracellular calcium release and interactions between myofibrils, eliciting contraction.
Does cardiac muscle require calcium?
The importance of calcium-dependent signaling in the heart has been appreciated for decades. For example, it is well accepted that intracellular calcium release from the sarcoplasmic reticulum (SR) is required for cardiac muscle contraction.How does calcium affect the muscles?
Calcium affects muscles by regulating contractions. This includes regulating the heart beating because the heart is a muscle that pumps blood. Calcium is released when a nerve stimulates a muscle. Calcium also plays a role in the complex process of blood coagulation (blood clotting).
Does calcium induced calcium release occur in cardiac muscle?
In cardiac muscle, a clear role in calcium signaling for calcium release from ryanodine receptors (RyR2) eliciting Calcium-Induced Calcium Release (CICR) is well documented.
What is the function of calcium in cardiac muscle fibers quizlet?
Calcium is needed to detach the myosin from the actin. Calcium is needed to allow the muscle fiber to become depolarized. Calcium is needed to activate troponin so that tropomyosin can be moved to expose the myosin-binding sites on the actin filament.
How does cardiac muscle contribute to the activity of the heart?
Cardiac muscle tissue works to keep your heart pumping through involuntary movements. … Your nervous system sends signals to pacemaker cells that prompt them to either speed up or slow down your heart rate. Your pacemaker cells are connected to other cardiac muscle cells, allowing them to pass along signals.How does increased calcium affect the heart?
Severe hypercalcemia can lead to confusion, dementia and coma, which can be fatal. Abnormal heart rhythm (arrhythmia). Hypercalcemia can affect the electrical impulses that regulate your heartbeat, causing your heart to beat irregularly.
What is the effect of calcium on heart rate?Heart rate was increased by calcium in the range from 1.6 to 14.0 mm and fell at still higher levels. A-V conduction time was shortest at calcium concentration slightly above normal, and decreased at higher as well as lower concentrations.
Article first time published onWhat is the role of calcium in excitation contraction coupling?
The calcium signals activate a contraction-relaxation cycle. Contraction refers to activation of the cross-bridge cycle. Ca2+ activates the attractive forces between the filaments of actin and myosin by binding to troponin (Figure 7-4).
How does low calcium affect muscles?
Muscle problems A person with a calcium deficiency may experience: muscle aches, cramps, and spasms. pain in the thighs and arms when walking or moving. numbness and tingling in the hands, arms, feet, and legs, as well as around the mouth.
Why is calcium release into the cytoplasm so important to muscle contraction?
Once stimulated, the sarcoplasmic reticulum releases calcium ions into the cytoplasm, where the calcium ions interact with troponin and remove tropomyosin from actin. This sequence allows for myosin to bind actin and shorten the sarcomere, resulting in contraction.
What is the role of calcium in muscle contraction quizlet?
What is the role of calcium in muscle contraction? Ca ions and proteins bond to actin play a crucial role in both muscle cell contraction and relaxation. … It binds to the troponin complex, causing tropomyosin bound along the actin strands to shift position and expose the myosin binding sites on the thin filament.
Why is calcium necessary for muscle contraction in other words what is the relationship between calcium troponin tropomyosin myosin and actin?
Calcium is required by two proteins, troponin and tropomyosin, that regulate muscle contraction by blocking the binding of myosin to filamentous actin. In a resting sarcomere, tropomyosin blocks the binding of myosin to actin.
What is the relationship of calcium to muscle relaxation?
Powered by ATP, it pumps calcium ions back into the sarcoplasmic reticulum, reducing the calcium level around the actin and myosin filaments and allowing the muscle to relax. Calcium ions are also used for signaling inside other cells, and similar pumps are found in the cell membrane of most cells.
Why is calcium not required for muscle contraction in this experiment quizlet?
Why is it not needed in the glycerinated muscle tissue? The glycernination process disrupts the tropinin/tropomyosin complex that otherwide blocks the myosin binding sites in living tissues, therefore no calcium is needed to induce contraction.
Does calcium bind to Calsequestrin?
Inside the SR, calcium is stored largely bound to calsequestrin, the only known protein dedicated to reversible ion buffering (1). In addition to storing calcium, calsequestrin has been proposed to mediate multiple functions (2).
What causes calcium to release from the sarcoplasmic reticulum quizlet?
Excitation refers to the release of calcium ions from the sarcoplasmic reticulum. Excitation, in this case, refers to the propagation of action potentials along the sarcolemma. … Excitation of the sarcolemma is coupled or linked to the contraction of a skeletal muscle fiber.
Why is calcium low in heart failure?
The cause-effect relationship between hypocalcemia and heart failure is based on the central role of calcium ions in myocardial contraction, which has been known since the early studies of Ringer in 1885.
Can high calcium cause low heart rate?
In the past, complications such as bone loss and fractures, kidney stones, kidney failure, hypertension and bradycardia (slowed heart rate), were commonly found as a result of longstanding untreated high calcium levels. These are now rarely seen thanks to blood tests that lead to preventive treatment.
What is the purpose of the cardiac muscle?
Structure and Function Rapid, involuntary contraction and relaxation of the cardiac muscle are vital for pumping blood throughout the cardiovascular system. To accomplish this, the structure of cardiac muscle has distinct features that allow it to contract in a coordinated fashion and resist fatigue.
What do the cardiac muscles do?
The muscle that makes up the heart is called cardiac muscle. … The thick muscles of the heart contract to pump blood out and then relax to let blood back in after it has circulated through the body.
How is cardiac muscle adapted to its function?
Cardiac muscle cells contract without stimulation by the central nervous system (contraction is myogenic) Cardiac muscle cells are branched, allowing for faster signal propagation and contraction in three dimensions. Cardiac muscles cells are not fused together, but are connected by gap junctions at intercalated discs.
How does calcium induced calcium release work?
Where does CICR occur in biology? During each heartbeat an influx of calcium through L-type voltage-operated channels provides the trigger to induce CICR from juxtaposed ryanodine receptors on the SR, resulting in cardiac muscle contraction.
Why does calcium unbind from troponin?
Voltage-sensitive dihydropyridine (DHP) receptors (L-type calcium channels) open to permit calcium entry into the cell during phase 2 of the action potential. … Unbinding of calcium from TN-C induces a conformational change in the troponin complex leading, once again, to TN-I inhibition of the actin binding site.
How do acetylcholinesterase and Ca2+ pumps function in the relaxation of a muscle?
How do acetylcholinesterase and Ca2+ pumps function in the relaxation of a muscle? Acetylcholinesterase degrades acetylcholine in the synaptic cleft, decreasing its effect, and consequently the excitation of the muscle fiber. Without further stimulation, calcium channels within the sarcoplasmic reticulum close.
What happens when the calcium Unbinds from the troponin?
If present, calcium ions bind to troponin, causing conformational changes in troponin that allow tropomyosin to move away from the myosin binding sites on actin. Once the tropomyosin is removed, a cross-bridge can form between actin and myosin, triggering contraction.
Why does calcium deficiency occur?
This deficiency may be due to a variety of factors, including: poor calcium intake over a long period of time, especially in childhood. medications that may decrease calcium absorption. dietary intolerance to foods rich in calcium.
What does calcium gluconate do to the heart?
Rapid intravenous injections of calcium gluconate may cause hypercalcaemia, which can result in vasodilation, cardiac arrhythmias, decreased blood pressure, and bradycardia. Extravasation of calcium gluconate can lead to cellulitis.
Why does low calcium increased excitability?
Hypocalcemia causes increased neuromuscular excitability by decreasing the threshold needed for the activation of neurons. As a result, neurons become unstable and fire spontaneous action potentials that trigger the involuntary contraction of the muscles, which eventually leads to tetany.